 To obtain health insurance, certain Medicaid enrollees may be subject to monthly premiums, the most common form of participation-related cost-sharing. State contracts with Medicaid managed care plans must follow the same federal regulations applicable under the state Medicaid plan, and they also must comply with specific regulatory requirements. Other federal regulations (issued October 1, 2013) address out-of-pocket costs for Medicaid beneficiaries enrolled in Medicaid managed care plans. This report includes examples of both types of beneficiary out-of-pocket spending in Medicaid. 7 States can use either Medicaid state plan amendments (SPAs) or Section 1115 waiver authority in the Social Security Act to establish both premiums and point-of-service cost-sharing. Medicaid premiums and service-related cost-sharing incurred by all individuals in a Medicaid household cannot exceed an aggregate limit of 5% of family income applied on either a monthly or quarterly basis, as specified by the state Medicaid agency. 5 Higher beneficiary cost-sharing is allowed in certain circumstances, and federal regulations modified some of these provisions. In SFY2013, 46 states (including the District of Columbia) reported having co-payment requirements. The cost-sharing amounts that can be charged vary with income. Some subgroups of beneficiaries are exempt from cost-sharing (e.g., children under 18 years of age and pregnant women). However, they cannot impose cost-sharing for emergency services or family planning services and supplies. States can also impose point-of-service cost-sharing, such as co-payments, coinsurance, deductibles, and other similar charges, on most Medicaid-covered inpatient and outpatient benefits. A survey by the Kaiser Family Foundation found that in state fiscal year (SFY) 2013, 39 states had at least one group able to participate in Medicaid by paying a premium, with a total of 59 different premium programs. However, premiums may be imposed on enrollees with income above 150% of the federal poverty level (FPL). In general, premiums and enrollment fees are often prohibited. 
States can require certain beneficiaries to share in the cost of Medicaid services, but there are limits on (1) the amounts states can impose, (2) the beneficiary groups that can be required to pay, and (3) the services for which cost-sharing can be charged. Today, participation-related cost-sharing (e.g., premiums) in Medicaid tends to be limited to certain subpopulations, and states use point-of-service cost-sharing more broadly. In July 2013, the Centers for Medicare and Medicaid Services (CMS) issued new regulations for Medicaid premiums and cost-sharing. 109-171) made additional, major changes to cost-sharing requirements that could be applied to Medicaid beneficiaries, including allowing states to permit providers to deny services when a co-payment requirement is not met. The Deficit Reduction Act of 2005 (DRA, P.L. 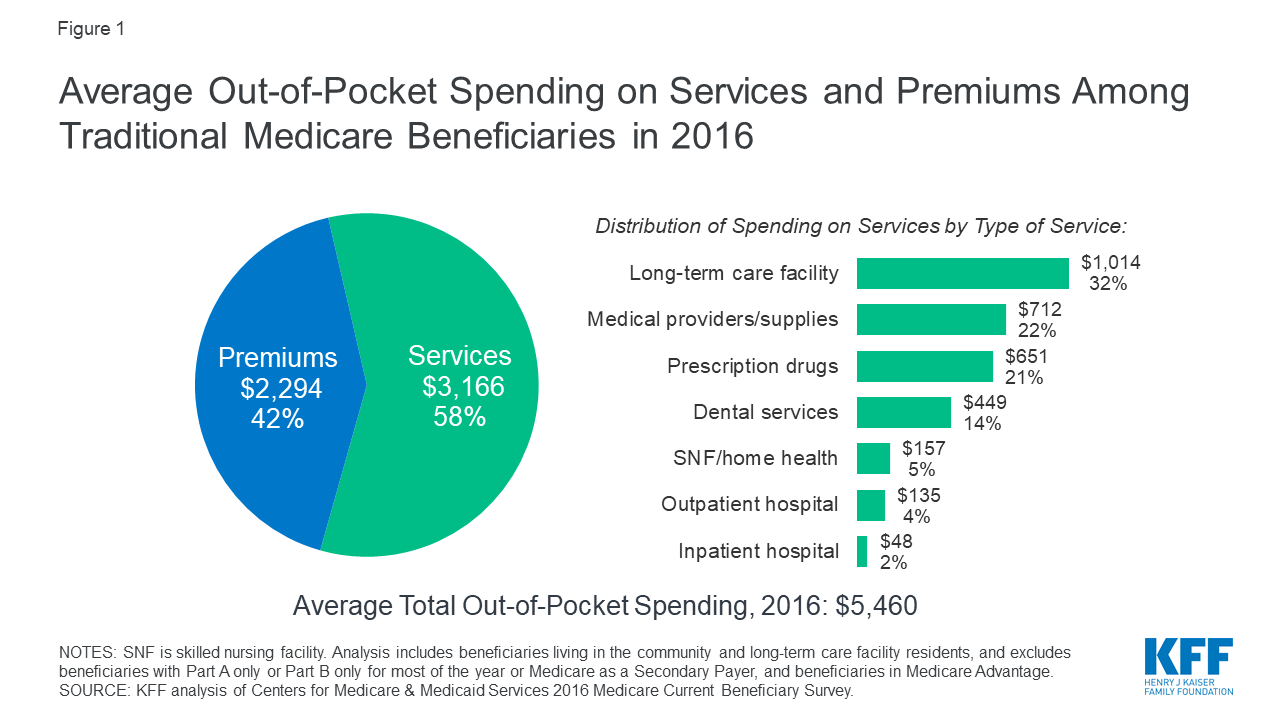
97-248, Subtitle B) added to the federal Medicaid statute the authority for states to impose enrollment fees, premiums, or similar charges as well as point-of-service cost-sharing. The Tax Equity and Fiscal Responsibility Act of 1982 (TEFRA 1982, P.L. Similar types of out-of-pocket cost-sharing can apply to individuals enrolled in private health insurance, although the amounts to which such beneficiaries may be subject can be higher than the amounts allowed in Medicaid. 
Cost-sharing requirements may include participation-related cost-sharing, such as monthly premiums or annual enrollment fees, as well as point-of-service cost-sharing such as co-payments-flat dollar amounts paid directly to providers for services rendered. As a result, there is significant variation across states in terms of who is eligible for coverage, what services are available, and which subgroups of beneficiaries are subject to out-of-pocket costs. 
1 Each state designs and administers its own version of Medicaid under broad federal rules. Medicaid is a means-tested entitlement program that, in FY2012, financed the delivery of primary and acute medical services, as well as long-term services and supports, to nearly 57 million people and cost states and the federal government a total of $431 billion. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
